 Jen and I decided to share some of the details of my daughter’s recent medical situation. We’re doing so because the condition is rare and as we were going through what I’m about to relate, we pored over the internet looking for any information that might fit the facts and help us solve Delaney’s problem. There wasn’t much, so we decided to put this out there as an aid to any parents whose child presents with similar symptoms. So….
Jen and I decided to share some of the details of my daughter’s recent medical situation. We’re doing so because the condition is rare and as we were going through what I’m about to relate, we pored over the internet looking for any information that might fit the facts and help us solve Delaney’s problem. There wasn’t much, so we decided to put this out there as an aid to any parents whose child presents with similar symptoms. So….
The Friday before Father’s Day in 2014, my two year old daughter and I were playing outside. She wasn’t quite herself, though, and eventually said she had a headache and asked to go inside. We did, she sat on the couch and seemed fine, and I didn’t think much about it until the next day, when she complained about pain above and slightly behind her right ear. Over the previous couple of weeks a vicious cold virus had flattened everyone in the house, so we feared she had developed an ear infection. We took her to the “doc in the box” at CVS and the nurse practitioner there diagnosed her with a double ear infection, prescribed an antibiotic, and off we went, thinking the problem would soon be solved.
The next day, Father’s Day, she woke with pronounced torticollis (head tilt) to the right and was screaming over the pain in the occipital area of her head (kind of above and behind her right ear). My wife immediately took her to the emergency room at a local hospital.
The attending physician in the ER was, in a word, an idiot. He checked her ears and said he saw no evidence of an ear infection (either the attending was wrong or the nurse practitioner from the day before was wrong, because the antibiotics would not have gotten rid of it in a day). He didn’t image her head or neck. Instead, he assumed the pain and torticollis was a muscle spasm (which can happen and is very painful in children) and then forcibly turned her head to see if she could, in fact, turn. She screamed in pain at this but did turn somewhat. This, in the attending’s mind, confirmed the diagnosis of muscle spasm. We took her home. But it was not a muscle spasm.
Oh, and here’s the thing for any parent whose child presents with torticollis: UNLESS YOU KNOW THE UNDERLYING CAUSE OF THE TORTICOLLIS, DO NOT FORCIBLY ATTEMPT TO TURN THE CHILD’S HEAD OR ALLOW ANYONE ELSE TO DO SO. IT CAN LEAD TO CATASTROPHE, EVEN DEATH, DEPENDING UPON THE UNDERLYING CONDITION.
The next day the excruciating episodes continued. The pain was intermittent, and the episodes lasted from a few minutes to a couple hours. It was agonizing. When the pain came on, she would scream, need to be held, and wanted to lay in her crib until it passed.
We put her on Motrin and Tylenol to help with the pain and called her pediatrician, who scheduled an MRI. At this point, the fear was a brain tumor. Thankfully it was not a brain tumor. The MRI was normal, but Delaney’s pain was unrelenting.
We stayed in close contact with Delaney’s pediatrician. Now, Jen and I can both be charming pains in the ass when we need to be, and advocating for our pain-stricken daughter probably made us a little less charming and a little more ass (or at least it did me), but so it goes. Sometime that week or next (my memory is fuzzy), the pediatrician sent us in for X-rays, looking for pharyngeal abscesses and other terrifying things. The X-rays were normal. At some point the pediatrician put her on a mild muscle relaxant. It did very little.
So we’re a couple of weeks into the symptoms and have an otherwise tough, precocious two year old in agony for much of the day, and no one seemed to have any idea what was wrong with her. The uncertainty and inability to do anything for her was heartbreaking.
Now, we’re fortunate to call a few doctors and hospital executives friends and neighbors, so we reached out. One of our great friends put us in touch with a senior executive at another local hospital, who, in turn, put us in touch with a pediatric neurologist who specialized in headaches in children.
She was wonderful but her exam revealed essentially nothing new. She confirmed that there’d been no neurological damage and suggested we try the muscle relaxant we were already trying. She arranged for a CT Scan of Delaney’s ear and an ultrasound of her neck, both of which would take place Saturday. The CT of the ear and U/S were both normal. We had nothing.
That weekend was terrible for Delaney and I peppered the neurologist with emails, telling her that Delaney was worsening and that we needed to do something. I think the Neurologist scoured the literature on these symptoms over that weekend and on Sunday she sent me a response, saying she wanted us on Monday to see a Pediatric Neurosurgeon and have Delaney evaluated for rotatory subluxation of her cervical spine.
I want to stop here for a moment, as the term “subluxation” sometimes calls to mind chiropractic medicine. Now, chiropractic medicine has its place, but (a) chiropractic subluxation theory (this is the theory that spinal subluxations cause anything from cancer to diabetes) is pure quackery, and (b) if your child has a rotatory subluxation of her cervical spine, DO NOT TURN HER OVER TO A CHIROPRACTOR FOR ADJUSTMENT. The potential for harm is enormous.
Anyway, we saw the neurosurgeon on Monday and, based on Delaney’s clinical presentation, he didn’t think she had a subluxation. She’d had no trauma, after all, and a two year old with a subluxation in the absence of trauma made little sense. Still, he eyed the MRI (which shows bone poorly) and thought maybe he saw an irregularity there. After consulting a radiologist, he decided to order a CT of the cervical spine to rule out a subluxation. We thought he would do this stat. Instead, for reasons we still don’t understand, it was scheduled for two weeks later.
Two weeks with my daughter screaming in pain everyday? That didn’t work for us. Friends helped us move up the appointment and we took Delaney in for the CT on Friday that week. After the CT, we were allowed to bring her home. The hospital called that evening, telling us to get Delaney back immediately because the CT showed a rotatory subluxation and she needed to be admitted. We did and she was.
We soon had a name for her condition — Grisel’s Syndrome. Essentially, Grisel’s is the non-traumatic subluxation of the atlantoaxial joint formed by C1 and C2. Basically C1 slides and rotates off of C2, causing the head to tilt in the direction of the slide. And in Delaney’s case, we think the subluxation also pinched the occipital nerve, which caused her agonizing pain behind/above her right ear.
So, if trauma did not cause this, then what?
In Delaney’s case, it was that upper respiratory infection I mentioned earlier. A cold. I shit you not.
It seems that in rare cases an upper respiratory infection causes inflammation in the tissue of the upper neck, causing the ligaments that hold the vertebrae in place to slacken. At that point, for some reason, and only in some children, the upper spine becomes vulnerable, and a sneeze, a cough, or a sudden jerk of the neck or head can cause a rotatory subluxation. That’s what happened with Delaney.
Now, rotatory subluxations come in four different types, type 1 through 4. The amount of displacement between the subluxed vertebrae is what determines the type. Delaney had a Type II or Type III, which meant there was a lot of displacement. She’d had it many weeks by then, and everything we read said that the longer the situation persisted, the more difficult it was to correct without surgery. Obviously we found this alarming.
But at least we knew what she had. We just needed to fix it.
Unfortunately, this situation appears to be rare enough that the protocol for treatment isn’t carved in stone. Worse, in this case the neurosurgeon we’d seen the first time went on vacation and handed us off to a colleague. This colleague seemed disinclined to do much of anything. For her first two days in the hospital the only treatment she received was a powerful pain reliever and a powerful muscle relaxant. At this point, the doctor was hoping the subluxation would self-correct (many do, but those are usually Type 1 subluxations, not IIs or IIIs). Part of the issue here was her age, which made some treatments difficult. Were she younger or older, they would have done traction. But they told us that traction was not an option for a two year old because she simply could not tolerate it.
We know now that this course of treatment was a mistake (she needed much more aggressive treatment and she needed it fast). But I think perhaps we accepted it because we hoped to have this fixed in the least invasive, least uncomfortable way for Delaney. On the third day in the hospital, the doctors put her in a soft collar. On the fourth day, they put her in a stiff cervical collar (an Aspen collar). No improvement. On the fifth day, they sent us home telling us that this could take “up to a month” to self correct.
Again, in hindsight, we learned that this was profoundly wrong. As I mentioned above, the longer a subluxation lingers, the more difficult it is to correct, short of surgery.
A couple weeks later (after one follow up appointment) we saw the neurosurgeon who’d seen her the first time (he’d returned from vacation) and he told us the subluxation had to be reduced (this is the medical term for realigning the vertebrae) as quickly as possible and proposed a “closed reduction.”
A closed reduction involves the child being completely sedated and the neurosurgeon pulling/manipulating the child’s head/neck in order to reduce the displacement. This is done while watching the bones move with an imaging device (in Delaney’s case a flouroscope).
Delaney’s closed reduction was a success, but the procedure only partially resolved the subluxation. It did, however, end her pain, which was a HUGE benefit. She continued to wear the stiff collar after the procedure and the doctor (it seemed) hoped that the now somewhat less displaced subluxation would self correct. An X-ray a week later showed that it hadn’t.
One week later we saw the neurosurgeon in clinic and had another CT. The subluxation had persisted and he offered us two options: Another attempted closed reduction followed by stabilization in a pin halo, or spinal fusion surgery. Of the two options, he seemed to think fusion was the best course. But Jen and I had decided that we would proceed with fusion surgery only if we had no other course (from what we’ve read and heard, and apart from the possible complications associated with the surgery, even a successful procedure would result in her losing 40-50% of the side-to-side rotation of her head).
We sought a second opinion. And a third.
And the third time was the charm. We consulted with a pediatric neurosurgeon at Mott’s Children’s Hospital at the University of Michigan and he suggested that it was too soon to jump to surgery. Instead, he recommended a closed reduction under CT observation, or traction via a pin halo followed by stabilization in a halo vest. If that approach didn’t work, surgery would be the only option left, but he thought the chance of success was good.
For a whole host of reasons, we found this a more desirable course. Delaney was admitted to the hospital again, sedated, and a pin halo affixed to her head via twelve pins. A traction device with a five pound weight was attached to the halo and she endured five days of that: unable to get out of bed, with a weight pulling her head upward. It wasn’t easy for her or her mom (who spent every night in the hospital) but they did it.
At the end of that period, a CT scan revealed that the subluxation had been reduced 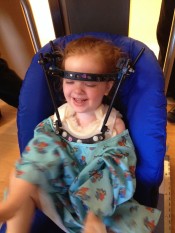 entirely. The ligaments would probably still be lax, of course, so she was fitted with a halo vest with rods, making it impossible for her to move her head. That’s where we are today. Essentially, it took two months from the onset of symptoms to get appropriately aggressive treatment. We hope it proves to be enough.
entirely. The ligaments would probably still be lax, of course, so she was fitted with a halo vest with rods, making it impossible for her to move her head. That’s where we are today. Essentially, it took two months from the onset of symptoms to get appropriately aggressive treatment. We hope it proves to be enough.
The halo vest will remain on for six to twelve weeks, after which she’ll continue to wear the stiff collar for a time. If there’s a recurrence, we’ll have to go to fusion surgery (because that would suggest ongoing ligament laxity which is too dangerous to leave alone). But we’re hoping there won’t be. Fingers crossed.
Meanwhile, this has done nothing to dim Lady D’s spirit (the girl is a spitfire) and she’s already tooling around in the halo like a crazy person (with Jen and I hovering around her to ensure she doesn’t fall or trip). So there’s that. 🙂
UPDATE:
Lady D wore the halo like a trooper for six weeks, then went to a rigid Aspen collar for a time after that. Follow ups show that everything remains in alignment. As of today, April 10, 2015, she is just a very active three year old. We’re soon to head to a water park and the doctors have told us it’s okay for her to go down the waterslides, but to exercise good judgement. Here’s D holding a copy of my latest book. 🙂


Sorry to hear about your child’s medical issue. Thoughts and prayers for a speedy recovery.
Thank you, Fred.
Please email me. My daughter got impetigo on her lip three little tiny dots. It turned into a deep neck abscess and almost took her life. Now we are awaiting additional scans because she has displacement of C1 and C2 and damage to transverse ligament.
Jennifer,
REsponded. Feel free to hit my wife and I with any questions. We’ll answer what we can.
My atlas subluxation is free after whiplash, however I have had open skin sores, constantantly gaveing to remove old skin
I don’t know you, or your family personally, but I do know you through Facebook and this site, and consider you and yours “family” in a way. I am so glad that Lady D is getting better and I wish her a very speedy recovery. As for you and the missus, you acted better that I would have. I commend you both, and hope that you never have to go through anything like this again. If you ever make it to NC, the Scotch and a cigar are on me. 🙂
Obliged, James.
I DO know your wife personally and I truly appreciate this in depth explanation of the hell your family has been enduring. Hugs and prayers to You, Jen & D, but also to the R’s & Baby S.
God Bless!
Love,
Mary A (from Burning Tree Lane)
Thank you, Mary. The support of Jen’s friends and family has been amazing. 🙂
Paul, your daughter is one tough cookie. When I got to meet her in person, the neck collar did not phase her. I watched in awe as she played as if everything was normal. She then snuggled up to me to watch a movie. I melted. I keep you all in our prayers and know what you wrote will help another parent diagnose much faster.
Thanks, Rena. 🙂
Your wife is the best, most heroic momma I know. Proud to call her a friend.
Bonus points for “I shit you not”. Nicely done.
“Your wife is the best, most heroic momma I know.”
Agreed. Delaney comes by her toughness honestly. 🙂
If she continues to need adjustment look into Spine Clinics. They do a computerized form of traction. Very complicated to explain but excellent theraphy. I have serve back and neck injuries from several accidents and falls and have been in debilating pain since 1988. I have been getting treatment 2 to 3 times a week for about 7 months. It is miracleous, My only regret is that I hadn’t learned about this years earlier. It is like getting my life back. Keep it in mind as a possibility before you resort to surgery.
Thanks, Shelley. And I’m glad to hear the therapy is working for you. 🙂
I have a two year old daughter myself. I’ve wondered how my wife and I would and should react when medical situations arise. I’d say you and your wife have given lots of us a good blueprint. You’ve got some prayers coming your way from Wisconsin. I wish your daughters recovery Godspeed.
Thank you, Jay.
Sorry to hear about the medical situation and the pain, wishing for the best recovery! But keep good spirits :D! Like the tiny crazy person, ah the joyful spirit of children :D.
Also will you file a complaint against the second doctor whom did not find anything?
Best wishes hope for the best!
Thank you, TB.
Paul,
I am so sorry your daughter and your family has had to go through all this. She certainly sounds like a tough little cookie.
Prayers for a speedy recovery.
–Eric
Thanks, Eric. Much appreciated.
As a parent with a very soon to be 3 year old I can’t imagine going through what you did. Hopefully, this post will help another parent in need. Thanks for sharing Paul.
Nick
Thank you, Nick.
Paul:
Hope your toddler recovers quickly and fully. Waiting for answers is hard to accept when it is your child. No parent handles the suffering of a child without being impacted themselves. One never expects a cold to have such impact on a loved one. My wife had a cold which attacked her heart. Luckily there is no significant ongoing effects. Peace be with you.
THanks, Tony.
As a pediatrician, it is heart wrenching to hear that it took 2 months for the correct diagnosis to be made and the appropriate treatment initiated. I am very glad, however, that her pain is gone and she is on her way to recovery. Thoughts, and will be following!
Thank you, Eric.
What a nightmare, Paul, for you and the whole family. Thankfully, Delaney’s on the mend, and she’s lucky to have persistent, determined, and intelligent parents looking out for her. Here’s to her healing fast and well.
Thanks, Matt. 🙂
Wow! 2 months of pain, and she is too young for whiskey!
All joking aside, I feel for your family, and am praying for a healthy and speedy recovery for your little one.
Thanks, Matt. Much appreciated.
You have gotten a ton of response already, but as a huge fan of your work and how you always give back to us fans, I wish you all the very best of luck for her. It’s hard enough as a parent to see your child hurting. It’s even harder when everything you do doesn’t help. My son went 3 days with a dislocated elbow as an infant as a 6 month old. Blame it on new parents or him being a total badass and barely crying. When we went to the er and they told us I felt terrible. This will pass and she will prevail. As always, may the force be with her and you. Not a religious man but I feel this is fitting to use in many a situation. Take care Mr Kemp. Hope all works out for you.
P.s thanks for Godborn. Finally got to read it. I needed Riven and Mr. Cale back in my life.
Thanks, Rodney. 🙂
Wow. Umm, SOOO sorry to hear about this terrible trauma, what a nightmare. Glad to hear your beautiful little girl is doing better. The solidarity and perseverance you and your wife showed for your child is absolutely sublime. I know from experience that when one’s child is ill yer pretty much constantly ripped on adrenalin, and it makes life difficult.
I just wanted to stop in and say SORRY, btw, a week or two ago I read about this on facebook and said something very insensitive, because I didn’t know you had a daughter, thought you just had boys, I thought this was some kind of medical thriller you were working on or some medical malpractice litigation you were working on instead of writing, which I made fun of, and you (rightfully) blocked me, I think. I AM SO DAMN SORRY, and yea I am that bonehead that comments w/o reading… /facepalm Also just wanted to say the last Cale book was THAT much better for having to wait so long to read it, I just finished it and it was SO DAMN GOOD, the scene where the protagonist meets Orsin….pure…energy. Thanks again for sharing your gift.
Clayton,
Appreciate the sentiment (and the explanation).
This whole ordeal must have been beyond terrifying and so frustrating, not knowing or being able to get help for so long. And very admirable of you to have the ability to think of others who might go through this by offering this piece to assist in finding help.
Glad to hear she’s doing better now – perhaps with her halo she should be ‘Angel D’? 🙂
P.S. Your Wikipedia link links to ‘Grisel’, not ‘Grisel’s Syndrome’.
Thanks and thanks, John.
Oh wow! Your poor little girl . What an awful ordeal for her and you to go through. Thank goodness she is on the road to recovery now.
My son was diagnosed with this syndrome last week. He has his tonsils and adenoids removed on the Wednesday and by Saturday he started to stoop. We just thought he was moving oddly due to the pain in throat and had a sore neck due to lounging around on the couch for a few days. We were going to take him to a physio on the Monday.
Luckily my husband ‘Googled’ sore neck as a symptom following tonsil removal and came across Grisel’s. As it is so rare, I told him there is no way our son would have it but luckily he didn’t listen to me and messaged my our son’s surgeon first thing Sunday morning. He was taken straight to hospital and fitted with an Aspen collar. Our son is the first patient his doctor has had contract Grisels and he has been removing tonsils and adenoids for nearly 40 years!
Luckily for us it looks like we got onto it nice and early and hopefully the Aspen collar will be off soon.
I hope your little girl makes a full recovery very soon.
Take care.
Fiona
Fiona, I’m so glad to hear you and your husband caught your son’s condition early on. That bodes very well for recovery (or so I’ve read).
As for D: The Halo has been off for two weeks now and everything remains in alignment. She’s been in the Aspen collar since. We’ve started to wean her from the collar now, per the doctor’s instructions. We’re hopeful!
I was so grateful that a good friend came across your blog, as our son was diagnosed with Grisel’s on Tuesday at UCSF. He had his adenoids removed on 4/20 and the following day would not lift his head up, he only moved his eyes up and he would not allow me to move his head back when washing his hair at all. I knew something was wrong and started calling his surgeon daily until on 4/28 they decided to x-ray his head/ neck, revealing a slight tilt in his spine.
He was put in a soft collar and given antibiotics right away. We are still here and I’m unsure of taking him home, as he is still unable to move his head up. Although the doctors have said the same, “they’ve never actually seen this and are researching as they go”.
After reading your blog I am going to ask for a properly fitted aspen collar, he’s a tiny 3 year old and there aren’t any soft collars small enough for him.
Our son has low tone or Hypotonia, it’s not uncommon but, after some of my own research, it looks like there could be a link to this condition. I read that children with lax ligaments are susceptible.
We are hopeful that we caught this in time for a full recovery but also want to be sure we are treating it as it should be treated.
You have been a big help in my research, thank you!
Christine,
I’m so sorry for you and your son. I hope all turns out well. It sounds like you got an early diagnosis and that’s a big deal. I’m very glad the blog was of some help.
I’m sure the specialists at UCSF are spectacular, but if, for any reason, you wanted the name of the pediatric specialists we dealt with at Mott’s Children in Ann Arbor (even if just to give the names to your docs at UCSF, perhaps for a phone consult), just email me at paulsvantekemp@yahoo.com. They Mott doctors seemed to have a great deal of familiarity with conditions of this kind.
Paul
My daughter Tayah had similar syptoms to your daughter. She is 5 and has been in her halo for 5 weeks. It took me from mid June 2014 to 5 weeks ago to finally get results and proper help. She had a pt hard collar soft collar valium botox injection chiropractor its been a long exhaustive road but finally a light at the end of the tunnel. Hopefully 1more week in the halo and were good to go.
Wow. Sorry to hear that, Melissa, but very glad to hear that things are on track with Tayah now. 🙂
This article is the one and ONLY article I have found that makes any sense to me! Thank you for that! The symptoms you describe your daughter as having, my son has been experiencing for over a year and not one doctor has actually addressed my concerns about this because my son also has several other health issues. He’s been complaining of pain behind his right ear which is worse during colds, but the ears look healthy (because it’s not ears and now I know!). He’s been complaining of neck pain for over a year and even saw a chiropractor for a short time. We couldn’t afford the chiropractor anymore and the pain then came back (started to go away with chiropractor). This weekend he had his adenoids removed due to sleep apnea issues and we had to take him to the ER for dizziness, nausea, horrible neck pain and stiffness. He was unable to move his head to the left or to look up. They said it was a mild onset of the beginnings of Grisel’s syndrome (and they called it a complication of adenoidectomy), but his x-rays looked good. So they put him an steriods to reduce inflammation and antibiotics as a precaution. Now reading your article I think that there’s a very, very real possibility that my son has been dealing with this issue for quite some time and that this recent surgery just made things aggravated. I now know what route I want to take to make sure extra steps are taken to address this issue! Thank you so much!!
Jamie,
I’m so glad the article was of help to you. I hope all turns out well with your son. 🙂
Hi! I suffered with this condition at the age of 11 and it took 18 months to finally diagnose! My parents were told it was muscle spasm and even that it was all psychological initially! Eventually I was offered a CT scan and then finally a diagnosis! After 6 weeks of traction and another 6 in a halo vest was told everything was normal! It was 10 years later when the condition came back when I was 21 and I then had fusion which was very successful! I am now 32 and although I do have reduced neck movement It is something I learnt to live with and I don’t notice even! I successfully learnt to drive and although have extra mirrors to help with vision am currently happy with the outcome! I just wanted to let you know that even years later the condition can reoccur as I am a living example! I would like to wish your daughter all the luck in the world and hope her treatment is successful!
After reading the blog and comments with great interest, I thought you might like to read about my experience of Grisel’s syndrome.
At 8 years old (I’m now 67) I developed an acute throat infection and very swollen neck glands, which were treated with penicillin injections. The swelling subsided within hours but I was left with my head twisted and tilted to one side and in great pain. I could neither raise nor lower my head without cupping it in my hands and ended up having to sleep in a sitting-up position. I was the eldest of 4 daughters (the youngest was only a 5-month old baby at the time) and when my condition didn’t improve the family doctor told my parents he thought the problem was psychological and that I was simply seeking attention. On his advice I was sent back to school, still in great pain and unable to turn my head. I still remember my young classmates asking me why my head was “crooked”, to which, of course, I had no answer!
It wasn’t until some 6 weeks later, after no sign of any change, that I was referred to a orthopaedic consultant at our local children’s hospital in the north of England, where X-rays finally revealed the subluxation (at the time this was explained to me in simple terms as ‘a dislocated neck’),resulting in me being immediately admitted to hospital, where I stayed about 6 weeks.
The year was 1956, long before MRI and CT scans. In those days the doctors referred to my condition by the umbrella term “torticollis” (it’s only since the advent of the internet that I’ve discovered it’s known as Grisel’s syndrome). My basic treatment consisted of time spent in traction, ultra-violet treatment, some nine months wearing a laced-up leather neck collar with a metal brace on the side towards which my head was tilted, and physiotherapy. At no time was surgery contemplated.
Those of you presently living with the uncertainty of the long term effects of Grisel’s syndrome, please take heart. Despite my case being one of late diagnosis in an era which didn’t have the benefits of today’s advances in medicine, I made a full recovery. Now, nearly 60 years later, I have absolutely no reduction in head or neck movement and no pain. My only physical ‘memento’ (which is visible only to me) is a very slight difference in the alignment of the ligaments on each side of my neck.
Hope my experience gives you some reassurance. A speedy recovery to all involved.
Thanks so much for sharing, Valerie. 🙂
Hi, our son has just been diagnosed with Grisel’s syndrome here in the England. They feared it was meningis at first. The hospital are in talks with the country’s largest children’s hospital today to discuss treatment. Thank you for publishing your account of events. Our little one is 5 and hopefully will stay to feel better soon.
Kind regards
My very best wishes to your son, Mark.
Paul…
I was doing a bit of research into Grisel’s this morning when I stumbled onto your harrowing story. Exactly fifty years ago I was in hospital traction being treated for torticollis as a result of an upper respiratory infection. The details of your daughter’s ordeal brought back a lot of memories (and, frankly, caused me to choke up a bit). It was all too familiar. It’s interesting to note that after fifty years, the treatment for Grisel’s Syndrome hasn’t substantially changed, only the diagnostics and tools for treatment have advanced. Anyway, all the best to Delaney in the future. She sounds like a very brave young lady. Peace and happiness to you and your family! MW
And likewise to you, Michael. Thank you.
I just wanted to say thank you for posting this. Our son had Grisel Syndrome in 2012 and was in halo traction for 4 months. He was diagnosed properly within a week, however treatment was incorrect (or lax) for nearly 2 months under the care of a paediatrician. I’ve been riddled with guilt over this since – why hadn’t I pressured the dr to fix it earlier while my son suffered? But reading your journey has comforted me. A rare syndrome can go improperly diagnosed or treated for so long. Thank you.
It’s crazy how often this gets missed. I’m glad you ultimately got your son the treatment he needed.
Thank you for posting the article about Grisel’s syndrome on your blog. Your story is all too familiar to me and my family now. My eight year-old daughter, Olivia, has had mistreatment after mistreatment in the Grand Rapids area following removal of her adenoids. Her symptoms began a few days after the surgery and persisted for months of pain, tilted neck, and intense muscle spasms while we were referred from doctor to doctor before an MRI was finally ordered that showed a subluxation involving C1 and C2. We will probably be getting the halo put on today, and we are praying for similar results. A closed reduction was tried yesterday and failed horribly. It took us three months to get here, and for the first time we feel like this could do the trick, but they are already talking about a fusion at GR Children’s Hospital because her condition has gone on for so long. Are you able to share the name of the neurosurgeon who you worked with at U of M? We decided we will be getting 3 or 4 opinions before moving forward with the fusion, and your story is promising.
Ryan,
Email sent.
Paul, can you or your wife please email me? Ametheney14@gmail.com
I have so many questions! My son recently had his adenoids taken out and tubes put in his ears. 2 days after surgery he started screaming in pain with his neck hurting him and said “head fall off” (he’s 2) with a headache. He has been living on Tylenol and motrin every 3/4 hours for almost a week now. Have been to Dr’s and e.r.s and just keep getting told it’s his muscles. One Dr had mentioned that his vertebrae had slid just a very tiny amount. Not enough to be concerned about and its not enough to cause this pain. But after reading your daughters story, I wonder. By the way, your daughter is absolutely precious. So glad she’s doing better!